Ptosis Repair Little Rock
Little Rock Oculoplastic & Facial Cosmetic Surgeon
Overview
Ptosis is a fairly common condition in which one or both of your upper eyelids droop. It is a common cause of reversible peripheral visual loss. Many patients with ptosis complain of difficulty with reading because the ptosis frequently worsens in down-gaze.
In addition, the visual field can be obstructed superiorly and laterally in many cases. Ptosis also can decrease the overall amount of light reaching the retina and therefore can reduce visual acuity, especially at night. Following ptosis surgery patients frequently note that they see better peripherally, have less trouble reading, objects look brighter, and the sharpness of their vision improves in many cases.
What Causes Ptosis?
Ptosis can occur in both children and adults. In some cases, it may occur during birth. Babies with ptosis must undergo a thorough eyelid examination.
In other cases, aging is the cause of ptosis. With advancing age, eyelid muscles and skin get stretched and become weak.
A previous eye surgery can increase the risk of weak eyelid muscles. This is because surgical instruments used to keep the eyelids away from the eyes during surgery can weaken the muscles.
Muscle diseases such as oculopharyngeal muscular dystrophy can cause weakening of eyelid muscles, leading to drooping. Ptosis can also occur over time due to an injury to the ligaments and muscles that control eyelid movements. Other reasons for ptosis include nerve problems, tumors, and infections in the eyelids.
Types of Pstosis
When discussing ptosis it is frequently helpful to classify the different types of ptosis. Ptosis can be categorized by onset: congenital or acquired. Ptosis may also be classified by its cause or etiology: involutional, myogenic, neurogenic, mechanical, or traumatic.
Involutional Ptosis
The most common type of acquired ptosis is involutional ptosis, which is usually age-related and result from thinning or disinsertion of the levator aponeurosis from its normal location.
Myogenic Ptosis
Myogenic ptosis occurs when the levator muscle is not made up of its normal healthy red muscular fibers but instead is somewhat fatty and fibrotic. The most common type of myogenic ptosis is congenital ptosis. Dr. Brock treats many children with congenital ptosis. Acquired myogenic ptosis can occur in diseases such as muscular dystrophy, chronic progressive external ophthalmoplegia (CPEO), myasthenia gravis (MG), myotonic dystrophy, or oculopharyngeal dystrophy.
Neurogenic Ptosis
Neurogenic ptosis can occur when patients have a palsy of the third cranial nerve. This is more common in diabetic patients and patients with hypertension. Sometimes it can be congenital. Another cause of neurogenic ptosis is Horner syndrome. Ptosis from Horner syndrome results when Muller’s muscle, a very small muscle located toward the back of the eyelid, loses its innervation. This can occur with some tumors in the upper lung, surgery on the carotid artery, or the condition can be congenital at times. Myasthenia gravis is another type of neurogenic ptosis that can simply be isolated to the eyelid. Usually with myasthenia gravis the eyelid function is worse when the patient is fatigued or in very hot weather. Myasthenia gravis may be ocular or systemic. Ocular myasthenia gravis can manifest with ptosis and intermittent double vision. Patients with systemic myasthenia gravis can have the ocular systems but also may have peripheral weakness and difficulty swallowing or breathing. In some cases this can be life-threatening.
Mechanical Ptosis
Mechanical ptosis usually refers to a condition when an eyelid or orbital mass is pushing the upper eyelid down.
Traumatic Ptosis
Traumatic ptosis can sometimes occur following eyelid lacerations, mechanical trauma from rubbing or having had other eye surgery.
Psuedoptosis (Apparently Eyelid Drooping
Pseudoptosis (apparent eyelid drooping) must be differentiated from true ptosis. Pseudoptosis can occur at times when the eyelid and/or brow weigh down the eyelid. With the excess skin and brow not weighing down the eyelid, the eyelid raises naturally.
Symptoms of Ptosis
The following symptoms can indicate ptosis:
- You are increasingly unconsciously lowering your face (looking down your nose), raising your chin, or raising your eyebrows to improve your vision.
- Your eyes appear smaller than usual because of your drooping eyelids.
- The fold that appears between the eyelid and eyebrow is no longer visible.
- Raising of the eyebrows is accompanied by headaches.
If ptosis is caused by a medical condition, then the above symptoms will be accompanied by symptoms of the underlying condition. For example, myasthenia gravis is a rare form of neuromuscular disease that weakens muscle response to nerve impulses. This condition weakens eyelid muscles, as well as the muscles of the face, legs, arms, and other body parts.
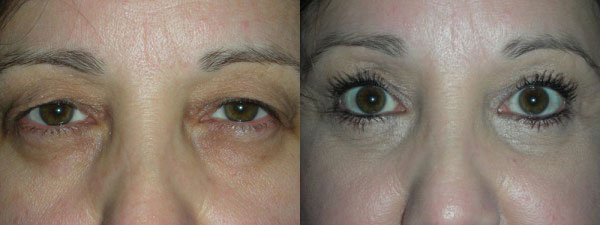
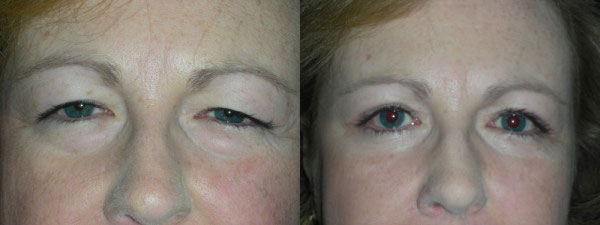
Photo Gallery
Before & After Photos
Ptosis Evaluation
When you arrive in our office and either you, your referring physician, or Dr. Brock has noticed that you have ptosis, we will want you to provide a medical, family, and surgical history. If your eyelids are obstructing your vision, you may be able to proceed with ptosis surgery as a medical indication. Each insurance company has local coverage determinations which must be met in order for your ptosis surgery to be considered medically necessary.
Your examination will include measurement of your visual acuity, measurement of eyelid height and function, and evaluation of your visual field (formal visual field testing may or may not be required), slit-lamp examination, and examination of your pupil and extraocular muscle function as well as photographs. If other factors besides the ptosis are discovered which could limit or alter the surgical plan, these will need to be addressed. An example of this would be a severe dry eye condition. An unrecognized or untreated dry eye symptom could result in possible postoperative concerns.
Dr. Brock performs ptosis surgery on hundreds of eyelids per year. He is very familiar with different varieties of ptosis and how they should be surgically approached. Because of Dr. Brock’s highly specialized skill in this area, facial and cosmetic surgeons all over the state regularly refer patients for routine ptosis surgery or also for patients who are at high risk of complications.
Ptosis Treatment Options
During a consultation, Dr. Brock will measure the degree of eyelid droop in order to assess the severity of the ptosis. Proper treatment depends on factors like the extent of functionality of the eyelid muscles. Ptosis can be treated successfully in the majority of cases.
Mild cases of ptosis where the patient’s vision is not impaired may need no treatment. If ptosis is impairing one’s vision or affecting their appearance, Dr. Brock will prescribe treatment depending on the cause.
Surgery is a common solution that can lift the eyelid back to its original position. This procedure is performed under local anesthesia and is quite effective.
In case of ptosis caused by an underlying condition such as an eye problem, muscle disease, or neurological disorder, treatment of the condition must take place before surgery can be performed.
Ptosis Surgery
Ptosis repair is generally performed with an external approach or internal approach. The external approach is the most common approach in Dr. Brock’s hands. The surgery is not performed under general anesthesia and is usually performed under IV sedation and local anesthetic. An external ptosis repair involves an incision in your upper eyelid crease. The muscle that elevates your eyelid, the levator, is identified and is either tightened or reattached, lifting the eyelid into a more normal anatomic position. The incision is closed with sutures that frequently are removed in approximately 7-10 days. Many patients may have some dermatochalasis (i.e., excess skin) and require blepharoplasty (i.e., removal of skin) at the same time as their ptosis repair. In addition, sometimes a patient’s brow may need to be addressed with a brow lift in order to optimize the outcome.
Surgical Techniques For Ptosis
External Approach
Ptosis repair with external approach: A skin incision is made through the front surface of the eyelid to reach the levator muscle and make an adjustment to that muscle. This may involve advancing the muscle or shortening the muscle.
Internal Approach
Ptosis repair with internal approach. The upper eyelid is everted and an incision is made on the back of the eyelid to adjust Muller’s muscle and lastly the levator muscle.
Frontalis Slin
Either a suture or the patient’s own fascia from the lateral thigh is used to connect the eyelid to the frontalis muscle above the brow.
Contact Our Office
To set up a consultation with Dr. Wade Brock regarding treatment for ptosis in Little Rock, contact our office today. Dr. Brock is a board-certified ophthalmologist and facial cosmetic surgeon with a great deal of experience, and he will be available to help you address your ptosis.
Testimonial
I absolutely love Dr. Brock and the entire staff at Arkansas Oculoplastic Surgery. While any type of surgery, especially involving the eye(s), can be concerning or frightening.